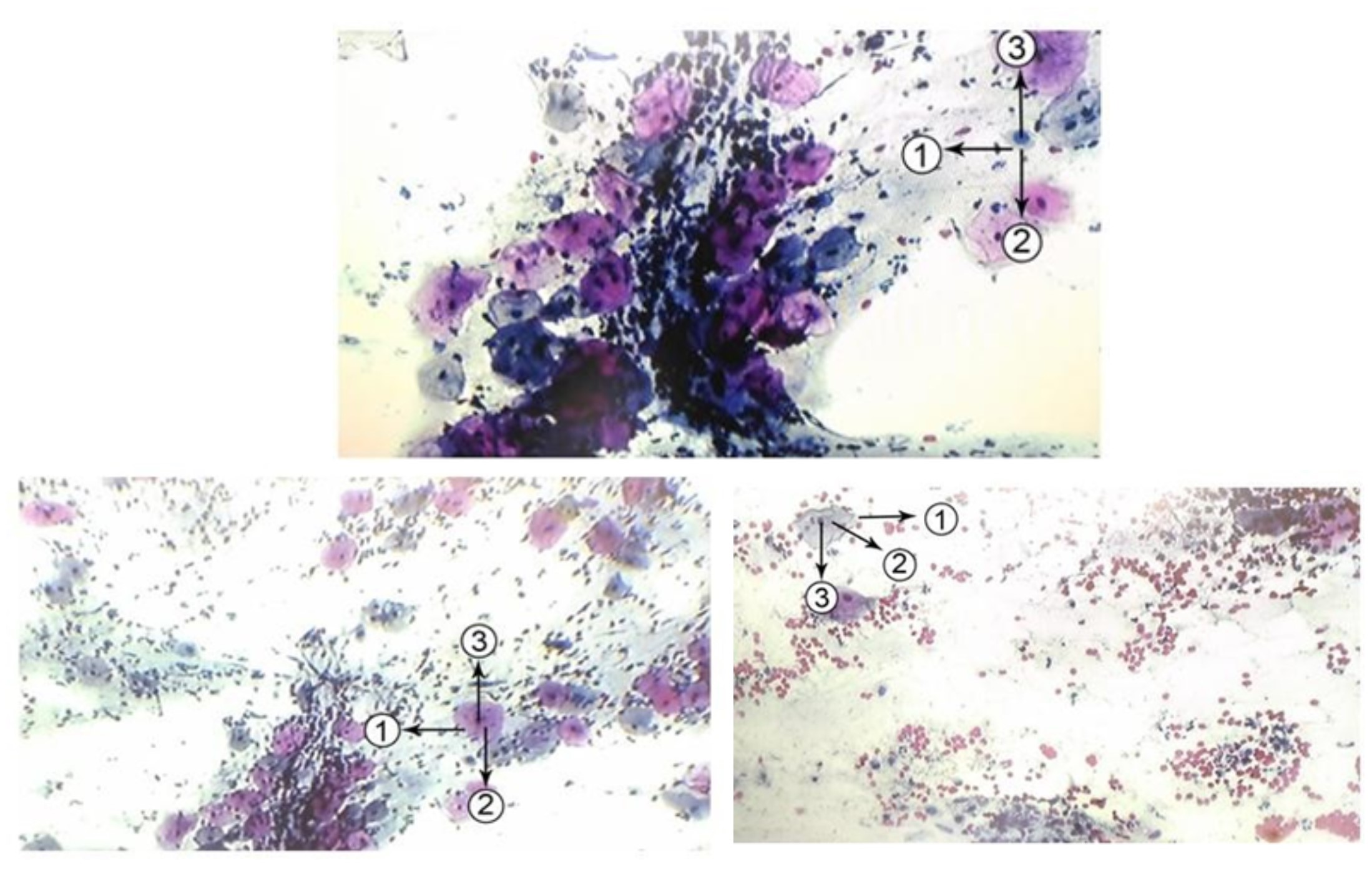
Comparison of Pap Smear Preparation Quality Containing Orange G and Without Orange G on the Results of the Papanicoulou Painting
Abstract
Examination procedure for pap smear preparation is influenced by fixation, drying and painting, and interpretation capability of examination. The Papanicolaou painting uses Harris Hematoxylin, Eosin Azure (EA) -50, and orange G. Orange G colors the orange matured and keratin cells Keratinizing-pink/orange cells. Chromatin in the nucleus will bind alkaline paint (hematoxylin) and cytoplasm protein will bind acidic paint (Orange G) and nucleus in the core will bind acid paint (EA 50) so that the cell will turn into pink with a blue core. The coloring stage according to procedure is using Orange G, but some PA laboratories do not use Orange G. The research goal is to know the comparison of pap smear preparation quality which contains orange G and without orange G towards papanicoulou painting result. The research type is experimental; the sample was 16 samples with two treatments namely coloring which using Orange G and without Orange G. The preparation quality which contains Orange G obtained moderate result of 12.5%, and good 87.5%. The preparation quality without Orange G was not good result of 6.3%, moderate 18.8%, and good 75%. The statistical test result of Chi Square and Kappa showed that the result was p>0.05 which means that comparison result of preparation quality which contains orange G and without orange G there was no significant difference.
References
Aldrich, S. (2020). Papanicolaou's solution 2a Orange G solution (OG 6). Merck KGaA, Darmstadt, Germany
Asthana, A.S.A. (2014). Comparison of the routine Papanicolaou staining technique with the rapid, economic, acetic acid, Papanicolaou (REAP) technique. IJMDS. 3(2) : 484-489.
Barut, M.U., Kale, A. & Kuyumcuoğlu, U. (2015). Analysis of Sensitivity, Specificity, and Positive and Negative Predictive Values of Smear and Colposcopy in Diagnosis of Premalignant and Malignant Cervical Lesions. Med Sci Monit. 21:3860–3867. Published 2015 Dec 10. doi:10.12659/msm.895227.
Choudhary, P., Sudhamani, S., Pandit, A. & Kiri, V. (2012). Comparison of modified ultrafast Papanicolaou stain with the standard rapid Papanicolaou stain in cytology of various organs. Journal of Cytology. 29 : 241.
Danico, J.L. & Sugiharto, S. (2019). Gambaran hasil pemeriksaan Pap Smear LBC dan Tes HPV untuk deteksi dini lesi prekanker dan kanker serviks di Rumah Sakit Medistra Desember 2015 – Januari 2017 .Tarumanagara Medical Journal 1(1):340-345.
Izhar, S., Kaur, R. & Masih, K. (2014). Efficacy of rapid, economical, acetic acid, Papanicolaou stain in cervical smears as an alternative to conventional Papanicolaou stain. Journal of cytology/Indian Academy of Cytologists. 31 : 154 .
Manuaba, I. G. (2005). Pap Smear Examination. In: Rusmi and Sari, L, Eds. Fundamentals of Gynecological Surgery Techniques. Jakarta. EGC.
Maria, C., Zahra, R., & Sara, P. (2013). Prevalence of cervical-vaginal infections in the pap-smear samples in Iran. Glob J Health Sci. 6(1):201–206. Published 2013 Dec 19. doi:10.5539/gjhs.v6n1p201
Mach, A.J., Adeyiga, O.B. & Di Carlo, D. (2013). Microfluidic sample preparation for diagnostic cytopathology. Lab Chip.13(6):1011–1026. doi:10.1039/c2lc41104k
Pawliszyn, J., (2012). Comprehensive Sampling and Sample Preparation Analytic Techniques for Scientists. Elsevier.
Raju, K. (2016). Evolution of Pap Stain. Biomedical Research and Therapy 3(2),490-500.
Richardson, L.A., Tota, J., & Franco, E.L. (2011). Optimizing technology for cervical cancer screening in high-resource settings. Expert Rev Obstet Gynecol.6(3):343–353. doi:10.1586/eog.11.13
Suvarna, S.K., Layton C. & Bancroft, J.D. (2015). Bancroft’s Theory and Practice of Histological Tecchniques. Ed8 .Elsevier.p.132-137.
Tan, S.Y., Tatsumura, Y. & Papanicolaou, G. (1883-1962): 2015. Discoverer of the Pap smear. Singapore Med J. 56(10):586–587. doi:10.11622/smedj.2015155.